PeriCor, co-founded by Hopkins Mechanical Engineering PhD student Justin Opfermann, won the Phase II Small Business Innovation Research grant from the National Institutes of Health for PeriPath, a novel device that obviates the need for open cardiac procedures in children. This grant will provide around $1.8 million to help the development of the device in order to make it commercially available.
PeriPath allows for safer ways to implant cardiac devices in pediatric patients. For adults needing a pacemaker, doctors usually make a small incision into a vein and feed a wire about 1 millimeter in diameter through it. This wire goes into the heart and can be attached to a pacemaker that is put into the chest.
The same procedure cannot be applied to children needing the same cardiac devices. A child’s veins are not big enough to get the same sized wire inserted. Surgeons need to cut open the chest through the ribs or through the middle of the ribs and put the wires onto the outside of the heart, requiring open-heart surgery.
In an interview with The News-Letter, Opfermann discussed how he recognized this as a major issue while working at the Sheikh Zayed Institute for Pediatric Surgical Innovation at Children's National Hospital.
“When I worked at the hospital, we were looking at pacemaker implantation in infants and after speaking to a number of doctors realized this was a very painful, invasive surgery,” he said.
Opfermann also noted that children who need a pacemaker will probably need multiple surgeries, which creates additional complications.
“Anytime you open the chest, the patient will heal with scar tissue that makes the next surgery more difficult,” he said. “Any way we can minimize the number of open surgeries is beneficial to the patient.”
Over the course of seven years, Opfermann created PeriPath with the aim of avoiding these open-heart surgeries and allowing these procedures to be done with a minimally invasive surgery. A minimally invasive surgery only needs small incisions, which reduces collateral tissue damage, minimizes pain and shortens recovery times. PeriPath will enable children to leave the hospital the day after their procedure as opposed to spending upwards of two weeks in intensive care.
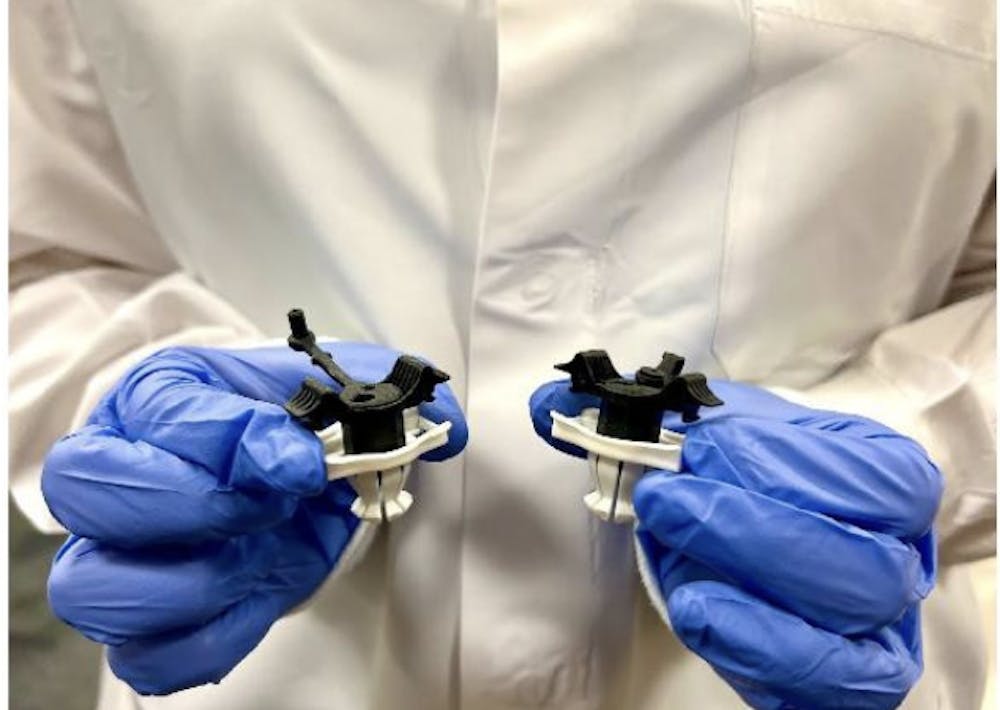
PeriPath works by allowing doctors to access the heart by going underneath the rib cage. Instead of needing to cut through the ribs, as done in open-heart surgery, going underneath the rib cage only requires a 1-centimeter incision and allows surgeons to implant the exact same pacing wires.
Additionally, the device’s design has two crossed channels: one for a camera and one for implant tools. This design properly aligns the implantation tools in the camera’s field of view, so doctors can see where the tools are in relation to the heart, which is another unique feature of this device compared to existing approaches.
Opfermann highlighted the importance and need for pediatric surgery devices because most people incorrectly assume that adult devices that are made smaller can be used for children. Additionally, there is less financial incentive to create pediatric devices.
“There are not as many pediatric surgeries, so unfortunately, companies may be disincentivized from developing pediatric specific solutions,“ he said.
Opfermann had a long, winding road to eventually creating a device in this field. Originally after studying Electrical Engineering as an undergraduate, he worked at General Electric. However, family situations led him to reconsider his career path.
“Early in my career, my mom was admitted to the hospital. When that happened, it made me rethink my career and how my skills could be used in another way,” he said.
This led him to go back to school to get a masters in Biomedical Engineering, specifically in bioelectronics. After this, he worked on cardiac devices at Medtronic and then started his own project at Children's National Hospital that led to PeriPath.
“Heart procedures are, one, very personal to me. But two, pacemakers are complex electronic systems that integrate with the heart, so it naturally fits my interests,” he said.
Opfermann plans to continue working on PeriPath while completing his PhD part-time in Axel Krieger’s lab at the Laboratory for Computational Sensing and Robotics. With the grant, he can work to get approval from the Food and Drug Administration to use his device in a clinical trial with human subjects.
He emphasized that there are many financial hurdles in getting this approval, such as manufacturing costs and a large array of tests proving its safety and efficacy.
“Finally, after seven years of development, we have the ability to complete a human study and that’s really been the end goal,” he said. “After we receive approval from the FDA, there will be a five-patient study at the Children’s National Hospital. That will be a life changing moment for those families and those children.”