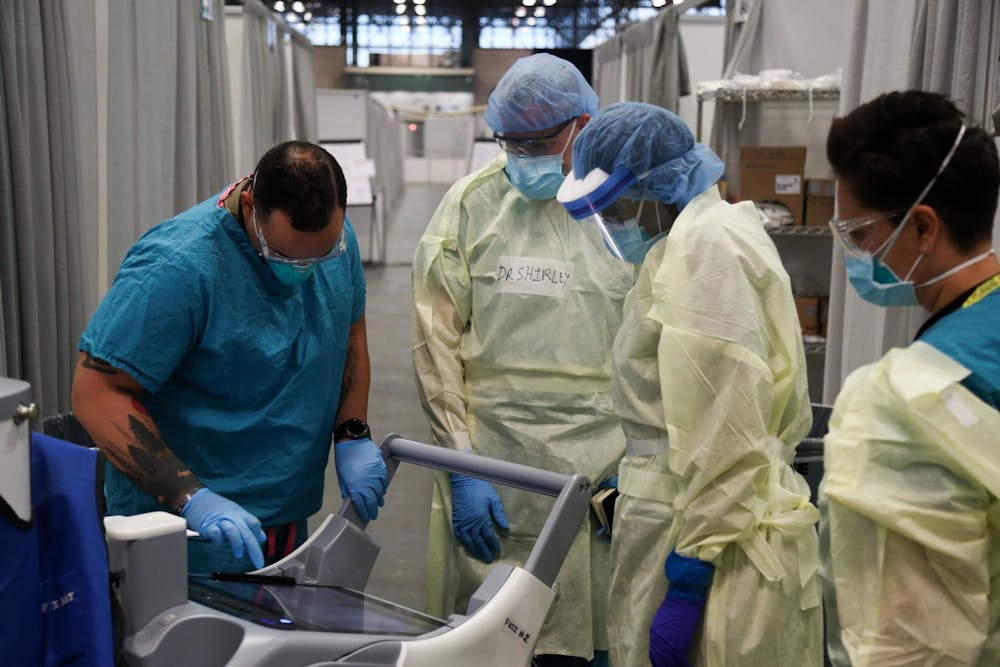
A survey was sent out recently to the Hopkins clinical research community to call for help with coronavirus (COVID-19) clinical research projects.
Dr. Daniel Ford, who is behind the survey distribution, is the director of the Hopkins Institute for Clinical and Translational Research (ICTR) and a member of the COVID-19 Hopkins Clinical Research Coordinating Committee.
In an interview with The News-Letter, Ford spoke about the reasoning behind the survey and the current state of COVID-19 clinical research at Hopkins.
Six months ago, there were no staff dedicated to COVID-19 research. As the epidemic turned into a pandemic, many more researchers and physicians are needed to combat the virus.
With non-COVID-19 clinical research projects halted, Ford explained that there is an opportunity to recruit staff from all areas of expertise — ranging from infectious disease, pulmonary division, general medicine and cardiology.
Ford and his colleagues on the committee are looking for experienced clinical researchers who would feel comfortable being in an in-patient environment with personal protective equipment. In general, the clinical research projects need help with drawing blood, collecting biospecimens, performing nasal swabs and obtaining consent for the biospecimens over the phone.
Ford explained that compared to nonclinical research projects, the clinical environment poses more risks. This is partly why they are being selective in who they allow to work in clinical research.
“We are hesitant to take any volunteers and put them into a COVID research situation with the patients,” Ford said.
Ford noted that there are also still chances for undergraduates to be involved. With proper training, biospecimen work and remote data analysis are possible ways undergraduates can contribute to COVID-19 research.
Still, some students do not feel qualified to participate in this manner. Senior Robert Medina, who has been involved in clinical research not related to COVID-19, explained his frustration of not being able to help in the current crisis.
“I realized that the clinical research that we were doing wouldn’t prepare me to handle the work demands of COVID research,” Medina said.
He wishes it were possible to be more involved with the University’s efforts to fight COVID-19.
“I think I would like to see opportunities where undergraduates can do lower level things to volunteer,” Medina said.
Though undergraduates are not currently serving in a clinical setting, physicians and researchers at Hopkins have been formulating ideas from all angles to approach the virus and design appropriate clinical research projects.
However, there is a limit to the number of COVID-19 clinical projects that can run at the same time, out of concern for patient well-being. Ford noted that the biggest concern for COVID-19 clinical research is to avoid inundating patients with an overwhelming number of tests and trials.
Most of the time, patients’ families are not allowed to visit due to safety concerns. Ford explained how it can be stressful for patients to have unfamiliar physicians asking them to participate in more clinical trials.
“We’ve tried to manage how many protocols there are, to assess their importance and make sure that our patients don’t get overwhelmed with choices,” Ford said.
The Therapeutic Pilot Committee within the ICTR is responsible for narrowing the proposals from approximately 20 down to only three at a time. Meanwhile, another committee is tasked with analyzing all patient data in the electronic medical records in order to ensure that patients do not undergo multiple testings for the same data.
Currently, there are about 25 approved protocols, with many more in the pipeline. Ford highlighted biospecimen projects as especially important. As an important part of the translational research, these projects correlate clinical and basic science research; in this case they connect patient data to the analysis of biological samples.
The highest priority for clinical trials right now is remdesivir, a drug which has received significant national and worldwide attention. Remdesivir is an unapproved antiviral drug which was first developed for Ebola and Marburg virus infections. As remdesivir shows antiviral activity against coronaviruses, more countries and scientists are running trials to test its effectiveness against the current virus. As of yet, there is no conclusive data that remdesivir works any better than standard care in treating COVID-19.
Hopkins is also conducting clinical trials on repurposed drugs, which are pharmaceutical products already on the market.
At the same time, clinical trials include much more than the conventional opinion of testing drugs or operating on patients. In the case of COVID-19, there is a clinical trial on the position of patients — lying on their stomachs versus lying on their backs — and their different responses. Another trial tests the effectiveness of drug administration through different means, via nebulizer or by intravenous injection.
Although the clinical testings of drugs are exciting and even promising, Ford warned of speculation over the preliminary results of any clinical trials. According to Ford, companies have been speaking to doctors and patients who are involved in clinical trials and asking for their “hunch” without any concrete scientific evidence.
In a world of manipulation and false evidence, Ford stressed that clinical trials must be randomized in order to determine the actual biological mechanisms of a drug.
“We have to be very careful in some ways not to give up on the scientific principles,” Ford said.