The Centers for Disease Control (CDC) recently reported that the number of attention-deficit/hyperactivity disorder (ADHD) medicine prescriptions for women increased nearly fivefold from 2003 to 2015.
Fifteen million adults in the United States have currently been diagnosed with the disorder. Additionally, men are three times more likely to be diagnosed than women.
Scientists believe that ADHD results from a chemical imbalance in the brain. A genetic mutation reduces the number of dopamine receptors in the brain, thereby preventing the so-called brain reward cascade from functioning properly. The brain, subsequently, produces less dopamine.
Dopamine is a neurotransmitter involved in producing feelings of pleasure as well as regulating attention in humans.
People with ADHD suffer from overstimulation, wherein they cannot block out irrelevant and distracting stimuli. They have trouble paying attention, get distracted easily and tend to be hyperactive. They also tend to be more impulsive.
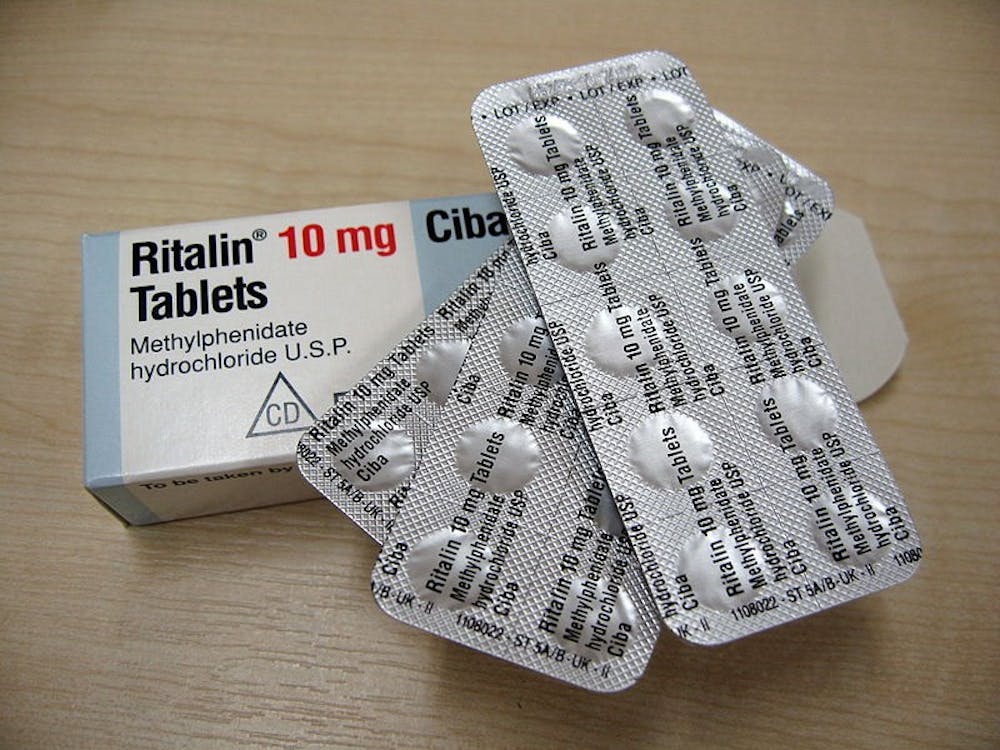
To treat ADHD, doctors prescribe psychostimulants that manage symptoms such as hyperactivity, interrupting and fidgeting. Common stimulants include amphetamine (Adderall) and methylphenidate (Ritalin).
In previous studies, researchers have determined that exposing a young animal to stimulants has a negative effect on its development. In humans, however, experiments have yet to elucidate the effects of stimulants on human pregnancies.
“Half of all pregnancies in the United States are unplanned, and women may be taking prescription medicine early in pregnancy before they know they are pregnant,” Coleen Boyle, director of the CDC’s National Center on Birth Defects and Developmental Disabilities, said in a press release. “Early pregnancy is a critical time for the developing baby. We need to better understand the safest ways to treat ADHD before and during pregnancy.”
Using the Truven Health MarketScan Commercial Database, a data set consisting of health insurance claims from a large sample of individuals with private insurance, the CDC identified changes in the numbers of reproductive-age (15-44 years old) women who filled ADHD prescriptions while pregnant over a 12-year period.
The percentage of reproductive-age women who filled a prescription increased over time for all age groups. The age group with the lowest increase in the number of ADHD prescriptions was 15-19 years old with an increase of 170 percent. The highest increase was between the ages of 25 to 29 with a 700 percent increase.
The study also analyzed the increase in prescriptions by geographic region. The greatest increase in prescriptions among reproductive-age women occurred in the South (380 percent).
The increase in the number of prescriptions filled by adult women corresponds with an overall increase in the total number of prescriptions filled in the United States among adults.
While ADHD symptoms typically emerge for the first time during adolescence, doctors have recently been diagnosing patients with adult onset ADHD as well.
One study, however, attempted to debunk this new form of the disorder, suggesting that if it exists, it is rare.
While the CDC study tracked the number of prescriptions filled, it did not take into account the patient’s symptoms that warranted that prescription.
Margaret Sibley, an associate professor of psychiatry and behavioral health at Florida International University and author of the opposing study, further shared her findings in a press release.
“If adult symptoms are being reported by patients, it shouldn’t necessarily be immediately classified as ADHD,” Sibley said. “A more careful evaluation often finds that there’s something else causing the problems, like depression, or drug use — which is what we found.”