A number of attempts to cure blindness in humans have emerged among researchers. The use of stem cells to aid regeneration of eye tissue as well as Vitamin A therapy for the treatment of retinitis pigmentosa, a condition that is characterized by the deterioration of the retina, are two possible cures for blindness.
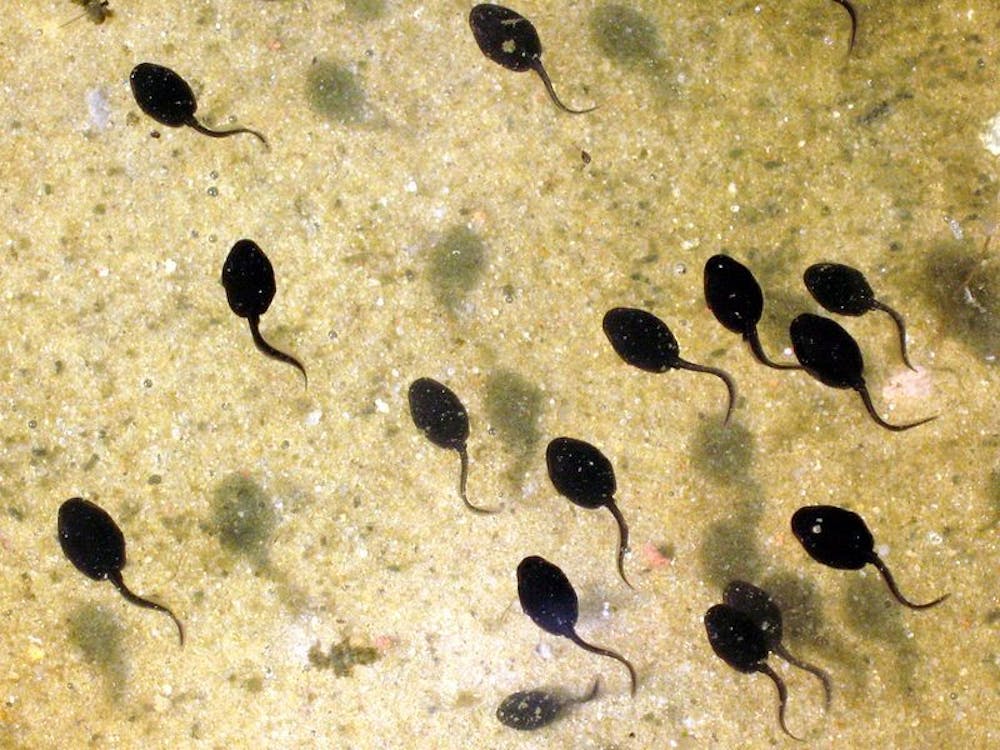
While these techniques have achieved some success at preventing blindness, they do not involve the transplantation of a visual organ onto the human body. Therefore, in an effort to comprehend the way in which an organism adapts to the regrown nerves from implanted body parts, blind tadpoles were studied as a model.
According to researchers from the Allen Discovery Center at Tufts University, the tadpoles demonstrated an increase in graft innervation when they were treated with a neurogenerative drug. Eyes were implanted on the trunk of the blind tadpoles’ tails before they were treated with Zolmitriptan, a drug that activates serotonin receptors involved with neural development.
Zolmitriptan is traditionally useful for alleviating migraines in humans, but the results of this experiment may reveal the effectiveness of repurposing neurotransmitters to benefit regenerative medicine.
To test the effectiveness of the eye grafting and the administering of Zolmitriptan, a series of trials was run. In the first set of trials, the tadpoles’ ability to distinguish color was examined by an assessment that entailed encouraging the tadpoles to occupy a blue space rather than a red space.
Out of the tadpoles studied, 76 percent without visual problems and three percent of blind tadpoles passed the assessment. Additionally, 11 percent of blind tadpoles that received implanted eyes and 29 percent of tadpoles that received both implanted eyes as well as the Zolmitriptan treatment passed.
“For regenerative medicine to move forward and enable the repair of damaged tissues and organ systems, we need to understand how to promote innervation and integration of transplanted organs,” Michael Levin, director of the Allen Discovery Center and Tufts Center for Regenerative and Developmental Biology, said. “This research helps illuminate one way to promote innervation and establish neural connections between a host central nervous system and an implant, using a human-approved small molecule drug.”
The tadpoles were also tested for true image-forming vision through their ability to match the direction of patterns rotating either clockwise or counterclockwise. An LCD screen above tadpole dishes was utilized to show the triangular clusters that moved every second.
The results of the image-forming test were as follows: 80 percent of tadpoles without visual problems and 38 percent of blind tadpoles passed the assessment. Additionally, 32 percent of blind tadpoles that received implanted eyes and 57 percent of tadpoles that received implanted eyes and the Zolmitriptan treatment passed.
“The fact that the grafted eyes in our model system could transmit visual information, even when direct connections to the brain were absent, suggests the central nervous system contains a remarkable ability to adapt to changes both in function and connectivity,” Douglas Blackiston, post-doctoral associate at the Department of Biology and Center for Regenerative and Developmental Biology at Tufts, said.
It is necessary for regenerated organs to establish connections within the body of an organism, especially when the implanted part has to do with the senses, so that there is an exchange with the brain of auditory, visual and tactile information.
The body’s ability to interpret visual inputs without clear connections to the brain is impressive, but the results from the use of Zolmitriptan solidify the importance of nerve regeneration in organ implants.
The research done in this study opens pathways for more innovation in how scientists can regenerate organs using different types of tissue. However, it is important to consider that the animal species used was the tadpole, so it may be some time before the findings can be applied to humans.
However, the research still shows that organ regeneration may not be limited to how many available donor organs there are. Patients may be able to use their own body parts to regrow a part of their body.













Please note All comments are eligible for publication in The News-Letter.